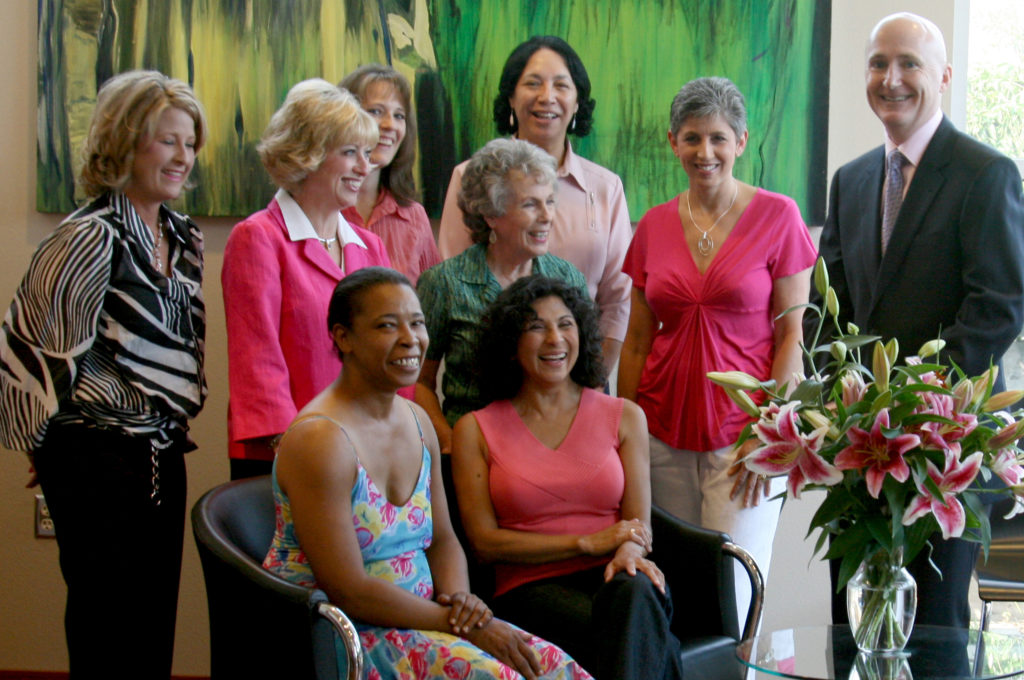
(Dr. Kunkel with some of his breast cancer patients)
One out of eight women in the United States will develop breast cancer. Breast cancer may run in families; a woman may be genetically susceptible to developing cancer. Reconstructing the breast(s) is often an appealing option. Breasts may be reconstructed using implants, a woman’s own tissues, or a combination of both. These procedures are almost always covered by insurance and can make an enormous difference is a woman’s self-image.
Dr. Kunkel has been doing breast reconstruction on women from Fort Worth, Arlington, Colleyville, Weatherford, and across North Texas for over 20 years. Fort Worth physicians have recognized Dr. Kunkel’s outstanding care of patients and have voted him a TopDoc (Fort Worth, Texas Magazine) 22 times! He has written a booklet about options for breast reconstruction and includes ‘Before and After’ examples of some of his patients. To see the booklet, click here.
Types Of Breast Reconstruction
There are a number of ways to reconstruct a breast. The best technique for any one person will depend on a number of factors. Your desires and expectations are important. Your health, age, and anatomical features play a role. The type, size, and location of the cancer also factor into the decision. The potential need for chemotherapy and radiation must also be considered.
There are two main types of breast reconstruction. The most common type uses some type of breast implant. The second type uses your own tissues to create a breast. This is called a “flap”, and there are several options. Sometimes a breast may require a combination of an implant and a woman’s own tissues. This can be a little confusing, and that’s why a visit with Dr. Kunkel is so important.
Breast Reconstruction With Implants
In 2016, 80% of women who underwent breast reconstruction had their breasts reconstructed with an implant of some type. Reconstruction with tissue expanders is the most common type of breast reconstruction in the U.S. Some women are candidates to skip the tissue expander altogether, however, and instead have the final implant placed at the time of the mastectomy. This is referred to as a “direct-to-implant” technique. Reconstruction with tissue expanders, as well as the direct-to-implant technique, are discussed below.
Breast Reconstruction With A Tissue Expander
This is the most common type of reconstruction. Breast reconstruction using a tissue expander is typically a two-stage process; at least two operations are involved. During the first procedure a temporary inflatable implant called a tissue expander is placed in the mastectomy site. Saline (salt water) or air is added to partially fill the tissue expander. Over the next few months saline is gradually added to the tissue expander when you visit our office. As saline is added to the expander the tissue stretches, or expands, creating a new breast shape. In the two videos below, watch as the nurse in the office shows how this is done.

Once the desired size of the breast has been reached, you undergo a second operation. The second procedure usually takes place 3 or 4 months after the mastectomy surgery. This second operation takes an hour or two and you go home the same day. The tissue expander is replaced with a more long-term breast implant. Most women choose a silicone implant, but saline implants are also an option. Additional adjustments may be made during this procedure as well. Sometimes an implant may require a little re-positioning. If a little more shape is desired at the top of the breast it may be possible to do liposuction of the abdomen and place that fat in the upper part of the breast (fat grafting). Insurance pays for all of this.
Dr. Kunkel has created a series of short videos of a tissue expander being placed in a woman immediately after her mastectomy. These videos are of a real patient undergoing surgery by Dr. Kunkel. If seeing actual tissues during surgery may make you uncomfortable, you probably should not watch these videos. If you are interested in seeing the videos, click here , then click on each of the videos that looks interesting to you.
Direct-To-Implant Breast Reconstruction

(Front and side images of a silicone gel breast implant)
It may be possible to skip the tissue expander entirely and just have the final implant placed at the time of the mastectomy. This is referred to as direct-to-implant reconstruction. Direct-to-implant technique creates the opportunity to complete the mastectomy and reconstruction in one operation. In many instances it even may be completed as an outpatient. You can undergo her mastectomy and reconstruction and sleep in your own bed that night! This is also referred to as “breast in a day” reconstruction. Some women, however, spend one night in the hospital.
Direct-to-implant reconstruction is a great option for many women, but some may not be candidates. For instance, sometimes the size and location of the cancer requires removal of a lot of breast skin. In cases like these, a tissue expander or use of your own tissues may be a better option.
Breast Reconstruction Using A Person’s Own Tissues: “Flaps”
An alternative to using implants is to use your own tissues. This may be a good option if you are generally in good health, near your ideal body weight, and you have not had a lot of surgery on your abdomen or back.
DIEP Flap
In DIEP flap surgery, breasts are made using your own abdominal tissues. This is a modification of an operation called a TRAM flap. TRAM flap procedures were common in the 1990’s and early 2000’s. As surgical techniques continue to evolve, DIEP flap surgery has replaced TRAM flap surgery in most situations. Skin and fatty tissue in the lower abdomen are removed and re-attached to small blood vessels at the mastectomy site. If you have had several abdominal operations you may not be a candidate for this procedure. If you have had multiple abdominal operations but still want to use your own tissues rather than an implant, there are alternatives. Sometimes tissue from the inner thighs or buttocks may be used instead.
Latissimus Flap Breast Reconstruction
In latissimus flap surgery, skin, fat, and muscle are transferred from your back to the mastectomy site. This tissue is draped over a tissue expander or an implant in the mastectomy site. Latissimus flap technique allows for more shaping and sculpting of the breast than just using a tissue expander or an implant alone. This may be a good option if your breasts are a little droopy and you are only going to have one breast removed. The skin, muscle, and fat create a more natural look and feel to the breast.
Nipple-Sparing Mastectomy/Reconstruction
In the past a mastectomy almost always required removal of the nipples. Advances in understanding of breast cancer and advances in surgical technique now allow many women to keep their nipples. Most women who have positive genetic tests for breast cancer are candidates for this type of reconstruction. A woman who has a small cancer located an inch or more away from the nipple may be a candidate. Dr. Kunkel works closely with breast oncology surgeons and medical oncologists to help identify the best candidates for this procedure.

(Dr. Kunkel and his Susan G. Komen Race for the Cure team)
What Is Oncoplastic Breast Cancer Surgery?
Many women with breast cancer choose to undergo a lumpectomy rather than a complete mastectomy. The advantage of a lumpectomy is that you get to keep your breasts. No implants are involved, and rarely is major flap surgery required.
In a lumpectomy procedure, when the breast oncology surgeon removes the tissue containing the cancer a defect is created. When an oncoplastic operation is chosen, Dr. Kunkel steps in and re-arranges adjacent tissues to fill the defect. In most cases this is much like undergoing a breast reduction or breast lift. Typically your nipple is elevated to an aesthetically pleasing position and the breast is re-shaped. This surgery is almost always completed as an outpatient. You go home and sleep in your own bed that night. Most women who choose this type of cancer care also require radiation.
What Is Recovery Like After Breast Reconstruction?
Recovery is different for women who undergo implant-based reconstruction (tissue expanders, direct-to-implant) than DIEP flaps. Women undergoing reconstruction with a tissue expander or an implant might spend one night in the hospital. It is possible to do the entire procedure as an outpatient; you may go home the same day. Here’s a short video showing a 67 year-old woman who underwent mastectomy and implant reconstruction and went home that afternoon. The video was taken the next morning when she came into the office for her first postoperative visit.
Most women are surprised at how good they feel and have little discomfort. Before the COVID19 pandemic, Dr. Kunkel urged his patients to go out and see a movie within 5 to 7 days of their mastectomy surgery. During the pandemic, he suggests patients stay at home for 7 days after their surgery but walk the neighborhood, get some sun on their face, and feel the great outdoors on their skin. You might be able to go back to work after two or three weeks, but no strenuous activity is allowed for about 6 weeks.
DIEP flap patients may spend 3 to 5 nights in the hospital or recovery center. In addition to your breast incision sites there are also abdominal incision sites and additional drain tubes. You will likely walk bent-over for several days. You may need additional help with dressing changes and physical activity compared to implant-based reconstruction.

(A patient of Dr. Kunkel’s two months after her cancer surgery.)
What Will the Scars Look Like After My Mastectomies?
Most women heal very nicely after undergoing mastectomies and breast reconstruction. A different incision pattern will be used in one woman compared to someone else. Each woman has her own unique physical findings and desires. Some women have previously undergone breast surgery like breast augmentation or breast reduction operations. Where a tumor is will also be a factor. Dr. Kunkel has created a video that talks about this. Take a look!
Nipple Reconstruction
It is possible to reconstruct a nipple, and there are a few options. Dr. Kunkel likes to wait to do nipple reconstruction until you are happy with the size, shape, and symmetry of your reconstructed breasts.
There are two major ways to reconstruct a nipple. If you want some projection of the nipple (front-to-back dimension), a brief 20 minute procedure is required. A small incision is made at the desired site for the nipple. Fatty tissue beneath the skin is pulled forward in that location. Small additional incisions are made to allow surrounding skin to be wrapped around the fat. This creates a small mound that looks like a nipple. About 6 weeks later color is added to the nipple and around the nipple to complete the reconstruction.
A different option is to skip the surgery and just have a tattoo. You decide where you think a nipple will look best on your reconstructed breast. You choose the color for the tattoo. The tattoo procedure is often done by a nurse in Dr. Kunkel’s office. It is possible to have this done by other tattoo artists as well, but most patients have it done in the office. These nipples can look very good, but there is no projection; they are flat like any other tattoo. The color may fade over time.