You have a job, you have kids, you have a life. You need to know what to expect after your cosmetic or reconstructive plastic surgery. Plans have to be made. What can you do after surgery, and how soon can you do it?
The answer to the question depends on how you heal. As a plastic surgeon, I can shape areas and put pieces together. Your body does the rest. It’s pretty cool, really. Your genetic make-up, your genetic code, is what determines how quickly and how well you heal. Of course, there are other influences. You have to “behave” after surgery, not doing too much too soon, or the incisions will pop open (insert sad face). If you love your dogs and cats and let them sleep on the same pillow as your facelift incisions will be resting on, infection may disrupt the healing process (insert ‘ewww’, and sad face). But in general, healing is all in your genes.
biology and wound healing

Have you ever been driving on I-30 or I-35 where they are doing construction on part of the freeway? First come the safety cones and warning signs, letting you know construction is ahead. Then you drive by an area where there are trucks leveling the ground. A little farther down the road a crew is laying rebar. Half a mile from there a crew is pouring concrete. When you drive by that area six months later the cones and construction crew are gone and you hum along at, ahem, the speed limit. That’s kind of how a surgical incision heals.
wound healing after surgery: days 1 and 2
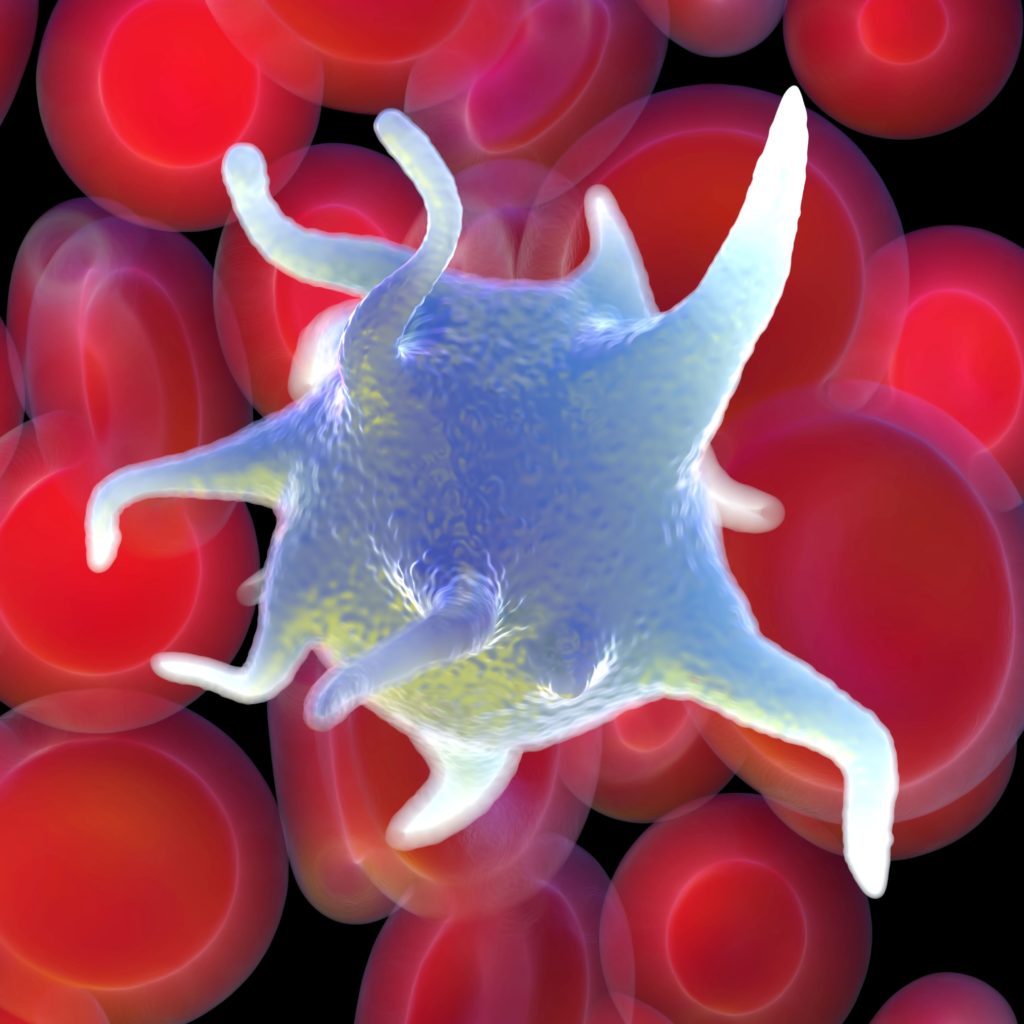
As soon as an incision is made, no matter how large or small, the body’s wound healing apparatus goes to work. It’s all pre-programmed. Within seconds your blood vessels constrict to reduce blood flow to the “injured” area. Cells called platelets (the white cell in the image above) stick together to seal breaks in blood vessels, forming little plugs. Those crafty platelets also release chemicals called growth factors. Some of those growth factors (PDGF, or platelet-derived growth factor, for instance) stimulate other types of cells to migrate to the injured site.

The cells we think of as the body’s “first responders” arrive in the first hour. These are white blood cells called polymorphonuclear leukocytes (PMN’s; the middle cell in the image above). PMN’s clear debris in part by releasing enzymes and free radicals. As this happens another group of cells called macrophages swoop in. Macrophages, like PMN’s, remove damaged tissue. And, just as platelets release growth factors, macrophages release their own special chemical growth factors. These factors (transforming growth factor beta (TGF), epidermal growth factor (EGF)) have their own roles. These chemicals stimulate yet another group of cells, called fibroblasts, to come check out what’s happening at the wound site. We’ll learn more about fibroblasts below.

wound healing: Days 3-14
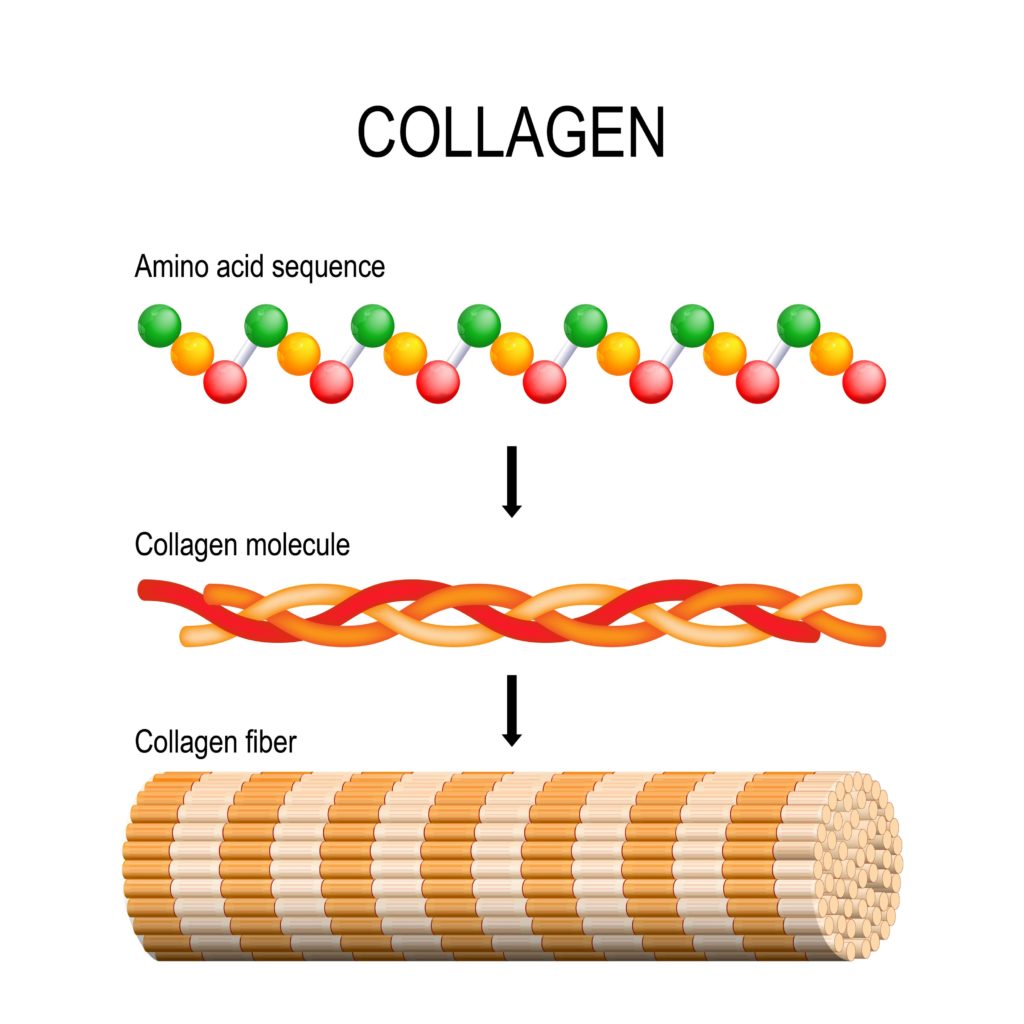
In the first two days bleeding stops and damaged cells and debris are being cleared away. On about the third day the all-important fibroblasts come in to lay the foundation for the wound to heal. Fibroblasts secrete collagen, and collagen makes the wound stronger. The collagen that your fibroblasts release in the first few weeks is different than the collagen your body makes later. The early collagen, called type 3 collagen, is disorganized and thick but definitely begins making the wound stronger. The number of fibroblasts releasing this collagen peaks at 7 to 14 days after the incision.
Other types of cells go to work around the end of the first week. Your body begins building new microscopic blood vessels in the area. Cells called epidermal keratinocytes proliferate at the edges of the wound and slowly begin migrating across the wound. Other cells (myofibroblasts) begin pulling the wound edges toward each other.
So, like happens in highway construction, different worker cells have been coming in on different days. Each type of cell is genetically coded to do a specific set of jobs at particular times, and this all happens without you even thinking about it.
By the end of the first week a wound has a little strength. That’s related to the collagen deposited by the early fibroblasts. The wound is really weak, though, not ready for your workout at Orange Theory or with your personal trainer.
Remember those epidermal keratinocytes? Those cells like to be kept moist. They don’t do well when they dry out. It’s for this reason that incisions may be covered with either tape or some other dressing that keeps them hydrated and moist. Sometimes antibiotic ointments help in prevent infection and keeping the incision moist during this time as well. Scar treatment gels and creams may also be effective. This is the time to use them. Don’t wait for six weeks. Start early. Of course, you should speak with your own surgeon about this if you’re not one of my patients!
wound healing: Weeks 3 to 6
Beginning in the second week, but really accelerating in the third week, the fibroblast cells proliferate and now secrete more type 1 collagen. Type 1 collagen is more mature collagen, more organized, and stronger than type 3. In the third week the collagen fibers begin to cross-link, adding more strength to the incision. The type 1 collagen fibers organize and form a 3-dimensional matrix that is stronger than individual collagen fibers. By the end of the fourth week, the wound is about 50% as strong as it is ever going to be.
So, with a wound that is 50% as strong as it is ever going to be after one month, are you ready to get back to kick boxing? Nope. Riding a bike? Maybe, depending on the situation. I don’t like for my plastic surgery patients to be athletically active at 4 weeks. Other surgeons may have other thoughts. The biology, however, tells us that your mommy makeover incisions really aren’t ready for prime time at the end of 4 weeks.
By the end of 6 weeks the concentration of strong type 1 collagen fibers is similar to that of normal skin. The wound is about 80% as strong as the tissues were before the incision was made, and that’s about as strong as it’s ever going to be.

I’m a little conservative when it comes to activity after cosmetic surgery. I tell my patients not to do strenuous activity for 6 weeks. At the end of six weeks, with the collagen having created a wound that’s about as strong as it’s going to get, I have patients get back to normal activities, including some athletics. However, I don’t want them doing the most strenuous activities that they do until the end of 8 weeks. There’s no real science behind that 2 week wait, however. To me it’s a matter of, you put a lot of money, worry, and effort into this operation. Why not wait a couple more weeks before going full tilt? The wound might be a little stronger then, meaning less chance of tearing something you don’t want to tear.
wound healing: beyond 6 weeks
Type 1 collagen fibers continue to organize for up to a year. That means that scars really aren’t ‘done’ for about a year or so. If you have a scar that’s a little raised or pink, keep on it. It may still respond to treatment.
what can i do, and when can i do it, after surgery?
That’s the question everyone wants answered. It’s just not possible to answer it for everyone, though. Each surgical procedure is different. For instance, liposuction is done through tiny poke holes in the skin. There aren’t big incisions to heal. A tummy tuck, on the other hand, is a much bigger operation and has much larger areas of tissue that have to heal. Similarly, breast augmentation is done through pretty small incisions, while breast lifts require much longer incisions.

Interestingly, we know that a little mechanical stress is required for normal wound healing. A little motion of a surgical wound accelerates the gain in strength of the wound. So, we actually want people to be ‘active’ after surgery. Just not too active. Being too active too soon may lead to an incision tearing open, or it may lead to worse scars. There’s probably a “Goldilocks” amount of activity allowable for each procedure, we just don’t know exactly what those are for which operations.
In general, I like for my plastic surgery patients to drive ‘sooner’ rather than ‘later’ after surgery. Of course, this depends on the specific operation being done. Breast augmentation patients might be able to drive one or two days after their surgery. Tummy tuck patients probably need to wait at least 7 to 10 days or more. Walking around the neighborhood? Go for it. Just don’t plan to climb steep hills or go up and down a bunch of stairs right away. We talk about activity level with each of our cosmetic and reconstructive surgery patients, and we relate that to the specific procedures. Each surgeon probably has her or his thoughts about activity level after surgery. If you’re not one of my patients, be sure to check with your doctor before doing anything discussed on this page. If you are one of my patients, we probably have already talked about activities. We just haven’t talked about the cells involved.
How you heal is already programmed into your body. Your platelets, PMN’s, macrophages, fibroblasts, and keratinocytes are there to serve you. You can help those cells by eating well, understanding what activities you should and shouldn’t be doing, and using scar treatments.
Biology is simply amazing!